When we have hurt our back, or have fallen and broken something, or have been in a car accident, or even been dealing with chronic pain… our go-to is to see our family doctor. Often, they will prescribe something to help:
- Muscle relaxers
- Anti-inflammatories
- Pain-killers
But what happens when the medication doesn’t “fix” the problem? Or if the issue we take the medication for keeps coming back?
Here is what is happening following an injury…
Recovery from an injury has roughly three stages. Timelines for each can vary based on the type of injury and degree of injury…
If medication is needed, most often it will be during the Inflammatory stage, and sometimes during the Repair stage.
Stage 1: Inflammatory
- As soon as an injury occurs, e.g. contusion or strain, tissues can tear internally as well externally (muscle fibers, blood vessels, bone break), etc.
- The injured area fills with blood but also inflammatory cells
- Any areas that are bleeding are quickly sealed off by special cells
- Classic inflammatory response of swelling, redness, heat, and pain occurs
- Physio Role at this stage: This is usually the time when we immobilize the area (e.g. bracing, splinting, taping, crutches)
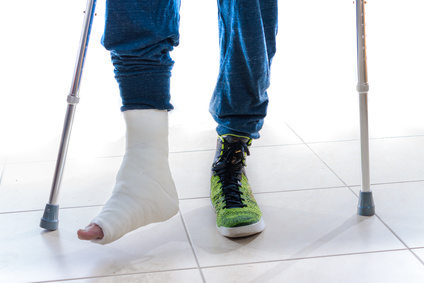
Stage 2: Proliferative / Repair
- Specific cells in the body are now clearing out the debris of dead tissue and dried blood
- Others are starting to create new tissue, including scar tissue
- Physio Role at this stage: This is the time to start gradually mobilizing the body in order to begin restoring range of motion, strength, proprioception, circulation, and to guide scar formation (scar tissue is laid down at random; use and movement is needed to guide which scar orientation is best for that particular part of the body)

Stage 3: Maturation / Remodelling
- The body continues to remodel the scar tissue
- New tissue is maturing into final stages of muscle, connective tissue, or bone
- Physio Role at this stage: This is the time to be returning to regular function and normalizing our biomechanics

Which is better, Physio or Medication?
This is like comparing apples to oranges. Physiotherapy and Medication often have different roles, with some general overlap. In the context of injury, medications seek to reduce pain, inflammation, and muscle spasm.
Physiotherapy seeks to do the same, along with returning to regular range of motion, strength, proprioception, and function. If the injury is something very minor with a short duration of recovery, Physiotherapy (or medication) might not even be necessary.
On the other hand, in more severe injuries, Physiotherapy might not be able to fully manage the acute symptoms…
Medication has a role to play in helping with excessive pain or muscle spasm, or with prolonged inflammation. Emphasis on “excessive” or “prolonged”, because after all, pain and muscle spasm serve a protective function to avoid further re-injury during a critical healing period. While the initial inflammatory response is part of the body’s healing process, when it’s prolonged it can hinder returning to function.
If you are already modifying your activity and avoiding undue strain, medication can help quality of life when the pain is unmanageable, and severely restricting your activity and work.
But, medication cannot make the damaged tissues stronger, or improve the mobility of a joint (unless the only thing limiting the joint movement was pain). This is where Physiotherapy comes in!
If I can do it with Physio, should I still take Medication?
It depends… are you doing alright without any medication, or are you having difficulty managing your symptoms even with the strategies suggested by your physiotherapist?
As explained above, medication can manage certain symptoms a lot better than Physiotherapy but does not address all factors necessary to get you back to your normal. It may have a role early on when symptoms are difficult to manage, but as your body continues to heal, that role should diminish.
In other words, the two can work well together, especially in the earlier stages when mobilizing and strengthening are impeded by pain, swelling, or spasm.
Talk to your Doctor about why they are prescribing the medication, what alternatives may be used (including Physiotherapy), and the pros and cons to both. Medication is not always necessary to get better, and it does carry side effects (especially if you are already on other long-term medications).
What about Medication for Chronic Disease?
This is a more complex question. Certain chronic diseases require pharmaceutical management and that’s okay. In fact, in some cases it is absolutely essential!
However, more recent research does show that medication for certain diseases can be reduced, or even stopped, with lifestyle changes! These lifestyle changes may be helped along with Physiotherapy, or other health disciplines, or you may gradually enact them on your own.

For example, changes in your eating habits and increasing your mobility can help you reach and maintain normal blood sugar levels, or manage your blood pressure, without the need for medication!
What about Medication for Chronic Pain?
When it comes to what Chronic Pain is, you can get more information from our previous Pain Series posts. The main takeaway, however, is that lifestyle changes are also key for management of Chronic (AKA Persistent) Pain!
Consider this… by nature, Chronic Pain has more to do with changes in the pain pathways and thresholds of the nervous system than with any recent injury. Since there is no recent injury that is responsible for the pain or spasm, and there is little value in an inflammatory response, medication that targets these issues is unlikely to be that effective. If anything, the longer you take it for, the more your body gets used to it and the greater dosage you will need. Not to mention the side affects added to the pain…
Ultimately…
Medication is reactive and often focuses on symptom management rather than addressing root cause. For certain chronic diseases, its role may be more complex and addressing the root cause may not be doable (e.g. genetic disease). But for others, like Type II diabetes, or high cholesterol, lifestyle changes can address the root causes!
Talk to your doctor about which medications are essential and which ones can be cut back with the right lifestyle changes. Come up with functional and recreational goals that are meaningful to you and talk to your physiotherapist about what activities and exercises might help get you closer to those goals!


