When we have pain, we often expect that imaging the area will tell us the cause. However, there tends to be a lot of controversy in the health care field about how helpful imaging actually is in the diagnosis of pain.
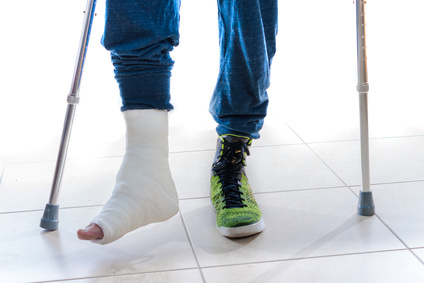
If you’ve had a fall resulting in…
- pain, swelling, bruising in the area
- difficulty with movement or weight-bearing
Then X-rays to rule out a fracture are important! Knowing early on if it is a fracture and the extent of it can dictate minimum the next 6-8 weeks of your treatment plan.
If you’ve hit your head and/or suffered a concussion with the following symptoms:
- weakness on one of side of your face or body
- difficulty speaking, hearing, or swallowing
- impaired vision
- seizures
- repeated vomiting
- one pupil is larger than the other
- severe headache
- loss of consciousness
Then, ruling out skull fracture and bleeding would be critical and time-sensitive!

Or, if you are experiencing any of the following “Red Flags”:
- loss of bowel / bladder control
- difficulty voiding either bowel or bladder
- loss of sensation in groin, genital, and anus areas
- unexplained weight loss / gain
Then, ruling out any serious causes would be critical and time-sensitive!
However, when the pain is more insidious and/or persistent, imaging results may not always give the most useful information…
What are the different types of imaging anyway?
Here we’ve listed the more common types of imaging for musculoskeletal (muscle, bone, general soft tissues) injuries:
X-ray radiography: X-rays are a form of electromagnetic radiation and are used primarily to detect bone fractures or degenerative changes. Can also pick up on certain tumours, pneumonia, calcifications, and foreign objects.
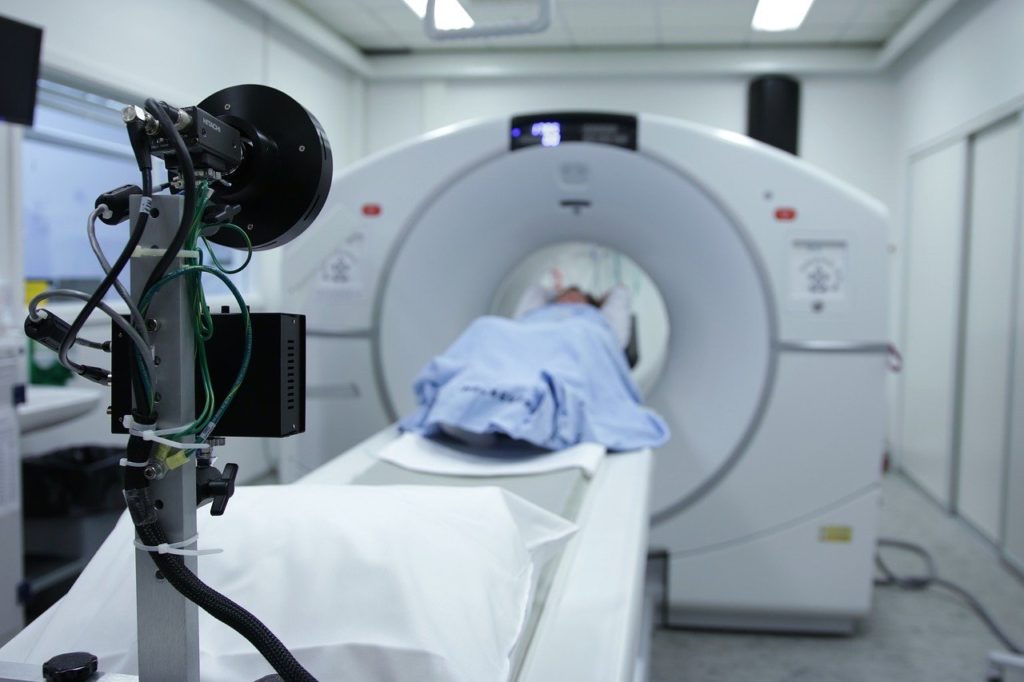
Computed Tomography (CT) Scans: combines X-rays with computer processing to get cross-sectional images of the body in order to form a 3D X-ray image. They are more detailed than regular X-rays and can show different angles of the imaged area.
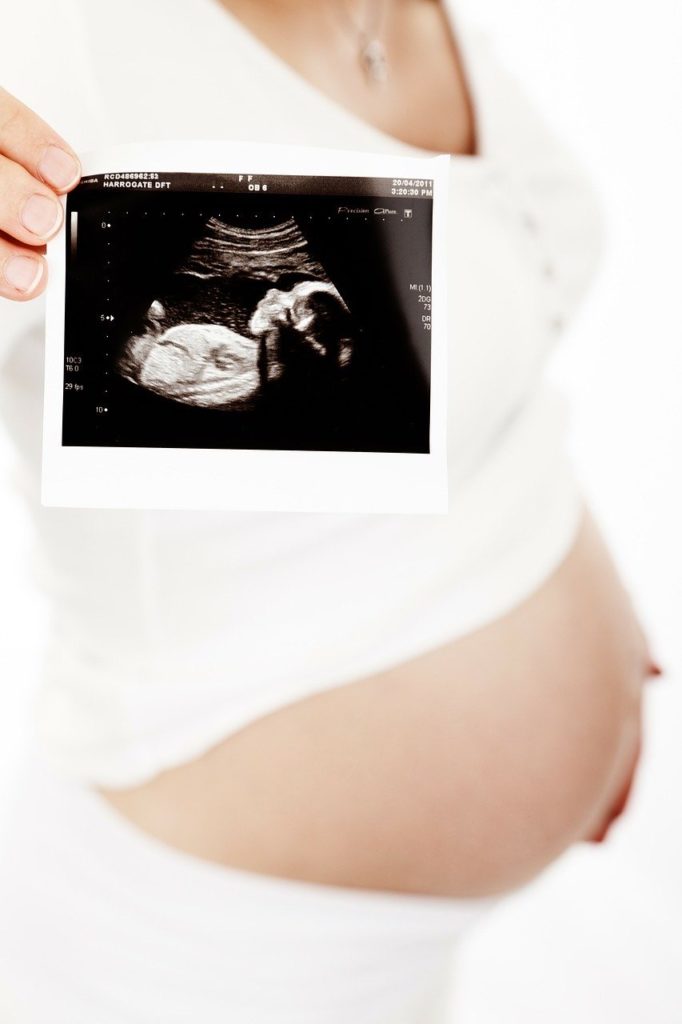
Diagnostic Ultrasound: Not to be confused with Therapeutic Ultrasound often used in Physiotherapy clinics, Diagnostic Ultrasound is a form of imaging using high-frequency sound waves. It is used for monitoring fetal growth during pregnancy, as well as visualizing organs (e.g. heart, liver, etc.), blood vessels, and soft tissues (e.g. muscles, ligaments). However, it is not good for visualizing bones or tissues that contain air (e.g. the lungs).
Magnetic Resonance Imaging (MRI): using powerful magnets, MRI machines are able to provide detailed 3D anatomical images. They are used to visualize bones and soft tissues in great detail. Unlike X-rays or CT, they do not use damaging radiation. However, the magnetic field is dangerous for people with implants, especially ones containing iron (e.g. pacemakers).
So why not get imaging just to be on the safe side?
Maybe you haven’t had a fall, or hit your head, but you still have pain. So why not get imaging just to make sure nothing is wrong? Of course you can, and oftentimes, that is precisely what doctors do.
But do not go into the lab expecting the imaging results to provide all of the information for why you have pain, or point you toward the best solution. Imaging is often only one puzzle piece in the diagnosis and solution, and sometimes it is not needed at all.

Based on your symptoms and their onset, your doctor may also weigh the risks associated with imaging. After all, if imaging is unlikely to provide useful information, is it worth being subjected to the radiation from X-rays or CT scans?
- Radiation from X-rays and CT scans increases risk of cancer
- X-rays and CT scans to the low back in child-bearing adults will expose the ovaries and testicles to radiation
- Imaging will often reveal benign abnormalities unrelated to the pain, which can lead to unnecessary worry, testing, and more invasive procedures

A lot of health care practitioners worry about what the effect of the imaging results have on the person on the receiving end.
Often, our imaging results begin to define how we view our body…
The language on the imaging reports can be harsh and difficult to parse out, because it’s laid out in medical terms and categories that are usually not explained to patients in terms of:
- what is normal,
- what it actually means for quality of life,
- how these results are influenced by our environment, lifestyle, or stress
- or, what symptoms can be reasonably expected based on these results
As a result, our story changes to one where our body is brittle and falling apart… when the reality is that our bodies are actually quite adaptive and resilient.

Maybe you have some experience with this… If you’ve had imaging in the past that has found some disc bulges and degenerative changes in your back, you might be more conscious of having a “bad back” and worry frequently about which activities you should avoid.
If you’ve had more chronic pain and recurrent imaging, think about whether or not the new images have ever shown much change in your joints or tissues, or given an explanation for a recurrence of acute pain. If not, perhaps you agree that there must be more to the story than just what the X-ray or MRI shows!
So today we will take some time to lay out the facts…
1. Degenerative changes in your spine, joints, and soft tissues are normal.
- After age 30, bone density begins to decrease, cartilage can thin, discs and ligaments and tendons become more rigid and stiff, and we lose muscle mass faster. This is why nutrition and exercise matter more as we get older.
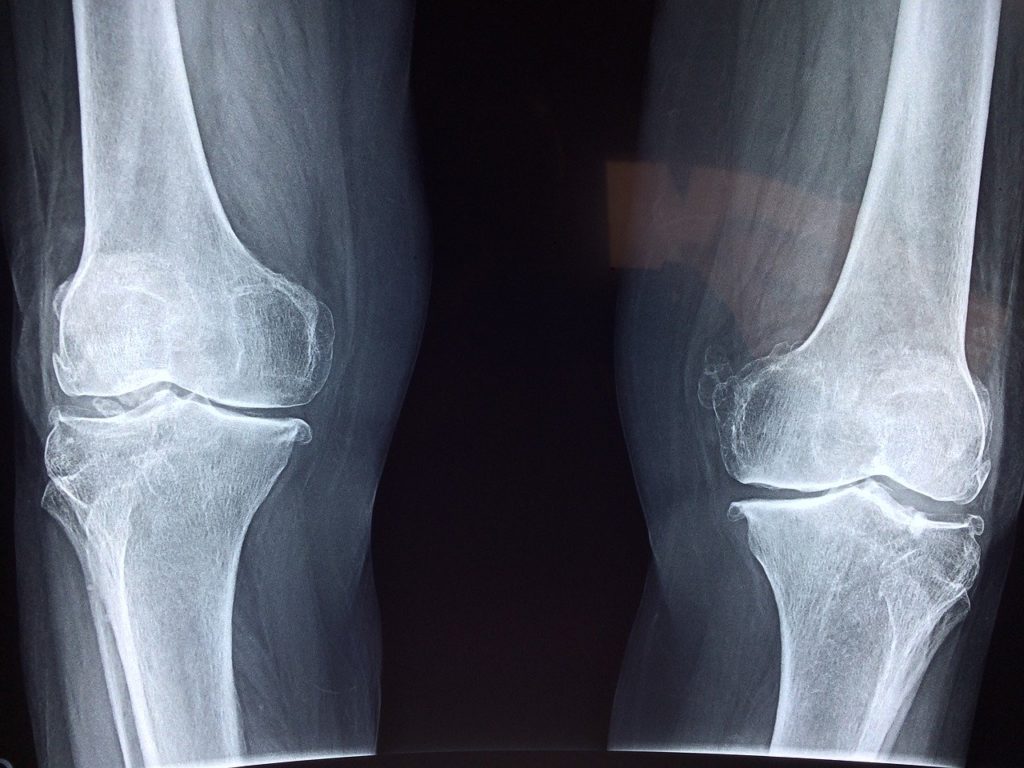
2. You can have degenerative changes (including disc bulges, rotator cuff tears, joint degeneration ranging from mild -> moderate -> severe) and have no pain!
- Imaging studies show that a high proportion of asymptomatic and healthy individuals can still have any of the above findings. E.g. Prevalence of disc bulges in asymptomatic 20-year-olds was found to be 30%! In asymptomatic 80-year-olds, it was 84%!
3. OA changes were present for a long time before your sudden onset of pain. While they may be contributing to the symptoms, they were not an issue before, which means that they are not the only factor to consider.
- Studies show that other factors have a significant impact on whether or not these OA changes become an issue (e.g. weight, muscle mass / strength, previous injuries, lifestyle factors including activity level and nutrition).
4. Disc herniations may not heal in the traditional sense, but it doesn’t mean they will always be source of pain!
- Eventually, they become asymptomatic as the inflammation and/or nerve irritation subside. Studies have also shown that herniated parts of the disc can sometimes be reabsorbed by the body so they are no longer an issue.

5. Almost all musculoskeletal injuries will heal between 3-6 months. Rehab for a fracture, such as the ankle, can take about 1 year. Which means that the persistent pain you may be experiencing has less to do with what you find on imaging, and more to do with other factors.
- Sometimes the nervous system can be a contributing factor to persistent pain. Check out our Pain Series blogs to learn more!
So what does all of this tell us?
Hopefully all of this information has given you a clearer insight into when should we image and why imaging isn’t everything. From this point on, take all imaging with a grain of salt and remember that it’s only a part of the puzzle, not the whole story!
If your imaging has shown degenerative changes, know that there are things you can do to help pain, quality of life, and focus on prevention. If you are having joint or muscle pain, if you have osteoarthritis, if you have nerve pain… ask us how we can help!

