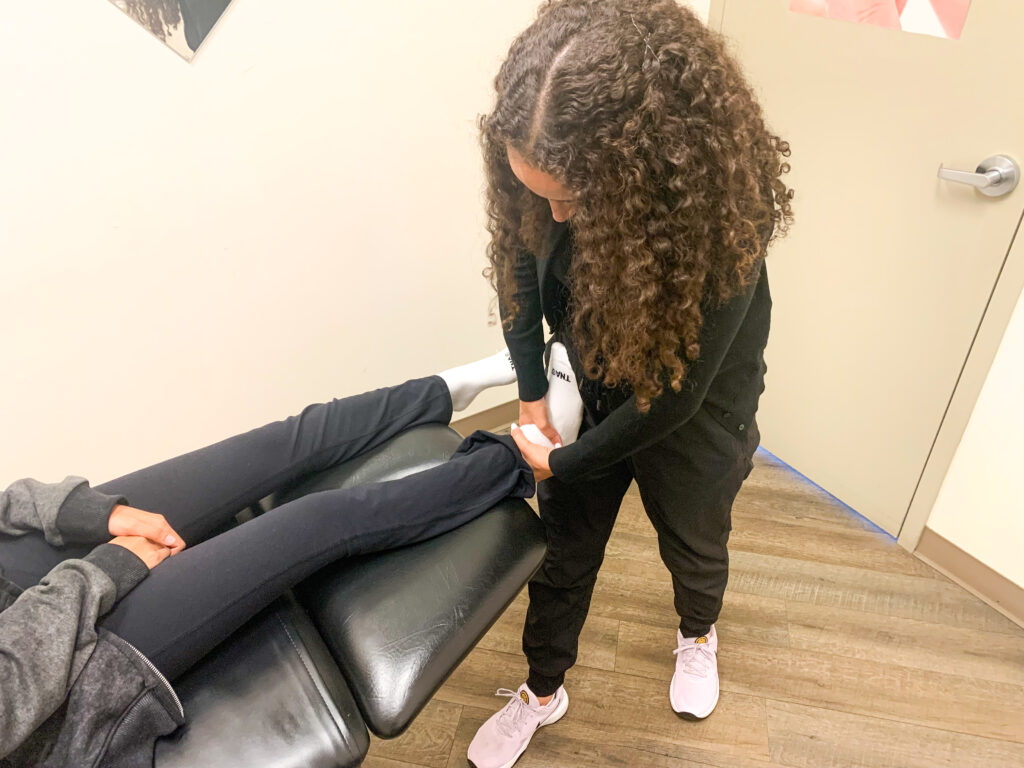
In today’s fast-paced world, workplace injuries are unfortunately all too common. Whether you’re working at a desk or on a construction site, every job comes with its own set of risks. However, there are proactive steps you can take to minimize these risks and keep yourself safe and healthy on the job. As your trusted physio clinic, we’re here to provide you with some invaluable tips for preventing workplace injuries.
1. Maintain Proper Posture: Whether you’re sitting at a desk or lifting heavy objects, maintaining proper posture is essential for preventing injuries. Sit up straight with your shoulders back, and make sure your workstation is ergonomically designed to support good posture. If you’re lifting, bend your knees and keep your back straight to avoid strain.
2. Take Regular Breaks: Prolonged periods of sitting or repetitive motions can lead to strain and injury. Make sure to take regular breaks throughout the day to stretch and move around. This not only helps prevent muscle fatigue but also improves circulation and reduces the risk of developing musculoskeletal issues.
3. Use Proper Lifting Techniques: Whether you’re lifting boxes in a warehouse or picking up supplies in an office, using proper lifting techniques is crucial for avoiding back injuries. Bend your knees, keep the object close to your body, and lift with your legs rather than your back. If something is too heavy to lift safely, don’t hesitate to ask for help.
4. Stay Hydrated and Nourished: Proper hydration and nutrition are often overlooked when it comes to preventing workplace injuries. Dehydration can lead to fatigue and decreased cognitive function, increasing the risk of accidents. Make sure to drink plenty of water throughout the day and fuel your body with nutritious foods to maintain energy levels and focus.
6. Stay Active Outside of Work: Engaging in regular physical activity outside of work can help strengthen your muscles, improve flexibility, and reduce the risk of injury. Whether it’s going for a walk, hitting the gym, or practicing yoga, finding activities you enjoy can help keep your body strong and resilient.
7. Listen to Your Body: One of the most important things you can do to prevent workplace injuries is to listen to your body. If something doesn’t feel right, don’t ignore it. Pain or discomfort could be a sign of an underlying issue that needs attention. Consult with a physiotherapist if you experience persistent pain or mobility issues.
At Palermo Plus Physiotherapy and Wellness Center, we’re committed to helping you stay healthy and injury-free, both in and out of the workplace.
If you have any questions or concerns about preventing workplace injuries or need assistance with rehabilitation following an injury, don’t hesitate to reach out to our team!
Stay safe, stay healthy!
Contact us!
Take the first step towards recovery by contacting us today or using our online booking system to schedule your initial acupuncture assessment and treatment.